Is Your Homecare DPDP Ready
1/8/20268 min read
Risk Analysis Report: Navigating Data Security and Liability in Home Healthcare under the DPDP Act
1.0 Introduction: The New Regulatory Landscape of Data Protection
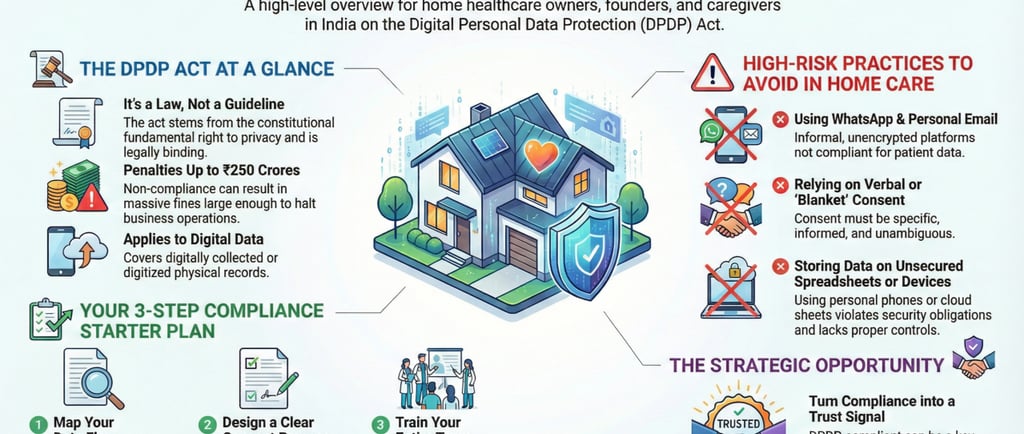
India's Digital Personal Data Protection (DPDP) Act marks a pivotal shift in the nation's legal landscape, elevating data privacy from a set of guidelines to an enforceable mandate rooted in the constitutional right to privacy. This new regulatory environment renders reactive compliance obsolete and demands a proactive strategy woven into the very fabric of operations for every organization handling the personal data of Indian citizens.
The DPDP Act is the legislative culmination of a journey that began with the landmark 2017 Supreme Court judgment affirming data privacy as a fundamental right. Its core philosophy is two fold: to empower individuals with clear rights and control over their personal data, and to fix accountability squarely on the organizations that collect and process it, known as "Data Fiduciaries." The law is designed to create a balanced ecosystem that safeguards individual privacy while enabling the continued growth of India's digital economy.
While sharing foundational principles with global regulations like the EU's General Data Protection Regulation (GDPR), the DPDP Act has distinct features tailored to the Indian context.
Parameter
DPDP Act vs. GDPR
Data Scope
The DPDP Act applies only to digital data, including physical records that are subsequently digitized. GDPR covers both digital and physical (paper) records.
Penalty Structure
Penalties are absolute monetary values, with a maximum of ₹250 crores. In GDPR, penalties are relative, calculated as a percentage of global turnover (up to 4%).
Definition of a Child
The DPDP Act defines a child as an individual below the age of 18, requiring strict parental consent. GDPR sets this threshold at 16 years.
This new legal framework presents unique challenges and significant liabilities, particularly for the home healthcare sector, whose operational model creates distinct data security vulnerabilities.
2.0 The Unique Vulnerabilities of the Home Care Ecosystem
To effectively manage risk under the DPDP Act, it is crucial to understand the specific operational context of home healthcare. Unlike a formal hospital environment, the home care sector is often characterized as informal, fragmented, and largely unregulated. This inherent structure elevates its data security risk profile, creating vulnerabilities that are often overlooked in traditional compliance models.
The fundamental operational challenge lies in the last-mile data collection process. Caregivers operating in informal home settings create significant "hidden grey zones" where sensitive patient information is gathered and transmitted through non-standardized and often insecure methods. This decentralized and uncontrolled flow of data stands in stark contrast to the structured information management systems found in hospitals, making home care organizations uniquely susceptible to breaches.
It is vital to clarify the scope of the DPDP Act in this context. The Act applies exclusively to digital data. This includes information collected directly in a digital format as well as physical records that are subsequently digitized—for example, a caregiver taking a photo of a handwritten paper form and storing it on their phone. While purely manual, non-digitized records are exempt from the DPDP Act, organizations must recognize that mishandling such physical data is not without consequence. It remains subject to other laws concerning breach of trust and can still expose the organization to legal action. As the expert clarifies, a patient can state, "I am your consumer... I can approach the consumer forum also."
Understanding this environment is the first step toward identifying the specific, tangible risks that emerge from these common operational practices.
3.0 Critical Risk Assessment: Identifying Key "Grey Areas" and Liabilities
This section deconstructs the common, often-overlooked operational practices within the home care sector and translates them into tangible risks and potential liabilities under the DPDP Act. The following analysis serves as the core of this risk report, highlighting the specific areas that require immediate attention and remediation.
DPDP Risk Matrix for Home Care Operations
Identified Grey Area
Associated Operational & Security Risk
Potential Liability & Financial Impact
Insufficient Staff Training and Awareness
Considered the most critical vulnerability, as untrained staff are the weakest link in data security. A lack of awareness about data privacy principles and legal obligations leads to unintentional but serious breaches.
Constitutes a failure of the organization's accountability obligations. A breach resulting from inadequate training can trigger the highest tiers of penalties under the Act (up to ₹250 crores).
Use of Informal Communication (WhatsApp, Gmail)
These platforms lack audit trails, access controls, and are not designed for medical data. They expose sensitive patient information to unauthorized access, interception, and uncontrolled dissemination.
A direct violation of the obligation to implement appropriate technical and organizational security safeguards, making a data breach highly probable and directly punishable.
Caregivers Using Personal Devices
Personal phones and laptops lack organizational security policies, access controls, and data leak prevention measures, making it impossible to secure, monitor, or delete patient data stored on them.
A clear failure to protect personal data. The organization is fully liable for any data breach originating from an employee's personal device, with no recourse against the employee under the Act.
Unstructured Data Storage (Excel, Google Sheets)
Storing sensitive patient data in spreadsheets with minimal security controls and no access logs violates data security obligations and complicates compliance with data rights.
Represents a failure to secure personal data and directly impedes the ability to honor a data principal's "right to deletion," making the organization non-compliant on multiple fronts.
Invalid Consent Practices (Verbal or Blanket Consent)
Verbal or overly broad "blanket" consent is not legally sound. The DPDP Act requires consent to be clear, specific, informed, and unambiguous for a defined purpose.
Processing data without valid consent is a foundational violation of the Act. All data collected under such consent is illegitimate and processing it can lead to severe penalties.
Lack of Data Retention/Deletion Policies
Indefinitely storing patient data without a defined policy violates the core principle of "storage limitation" and infringes upon a patient's right to have their data erased upon request.
Failure to honor a "right to deletion" request is a punishable offense. The absence of a retention policy signals a fundamental gap in the organization's compliance framework.
Insecure Data Sharing (Email, USB drives)
Sharing sensitive data via unencrypted email or physical drives creates an unmanageable risk of data loss or theft, with no ability to track or control the information once it has been shared.
This is a textbook example of failing to implement appropriate security measures to prevent a data breach, placing direct and severe liability on the organization.
Unvetted Third-Party App Usage
Using technology from vendors without a formal data processing agreement exposes the organization to risks from the vendor's security failures, for which the organization remains accountable.
The organization (Data Fiduciary) remains ultimately liable for any breach caused by its vendor (Data Processor), making due diligence and contractual safeguards essential.
Each of these grey areas represents a significant operational failure. Under the DPDP Act, the liability for a breach originating from an employee's personal WhatsApp is legally indistinguishable from a direct server hack—and the penalty, potentially ruinous enough to halt operations, rests solely with the organization.
To manage this liability effectively, it is essential to first understand who the law holds accountable.
4.0 The Principle of Accountability: Defining Roles and Responsibilities
A clear understanding of the legal roles defined by the DPDP Act is critical for effective risk management. The Act establishes a precise framework of accountability by designating two key entities involved in the data lifecycle: the Data Fiduciary and the Data Processor.
The Data Fiduciary
The Data Fiduciary is the primary entity that determines the purpose and means of processing personal data. To be clear: if you are a home care organization collecting patient data, you are the Data Fiduciary. The law places the primary burden of compliance directly on you. This is the most critical role, as the Data Fiduciary holds the primary legal liability and accountability for protecting personal data across its entire lifecycle.
The Data Processor
The Data Processor is any third-party organization that processes personal data on behalf of the Data Fiduciary. A common example is a technology company providing a software platform or a cloud storage provider. While a Data Fiduciary can transfer specific responsibilities to a Data Processor through a formal contract (e.g., ensuring data is encrypted on a server), the ultimate accountability for a data breach remains with the Fiduciary. If a vendor's system is breached, it is the home care organization that will face the legal consequences and penalties.
With a clear understanding of this liability structure, organizations can now focus on the practical, actionable steps required to mitigate these identified risks.
5.0 Strategic Mitigation Framework: Proactive Steps for Compliance
This section provides an actionable roadmap for home care owners, operators, and IT managers. While the penalties for non-compliance are severe, the path forward is straightforward. As the expert advises, the focus should not be on panic but on process: “it's just about following the guidelines... government is is not going to penalize to collect the money from you... it's just a a a strict request to follow not more than that.” Adopting this pragmatic mindset is key to building a compliant operational framework.
Map the Complete Data Flow The first and most critical step is a comprehensive audit of your organization's data lifecycle. Meticulously identify what personal data is collected (name, health conditions), how and by whom it is collected (caregiver on a mobile device), where it is stored (cloud server, local device), and with whom it is shared (labs, hospitals). During this process, tag all Personally Identifiable Information (PII), including names, contact details, and even IP addresses. PII can be a single piece of data or a combination. As the expert notes, there may be many 'Sujit Katiars,' but a 'Sujit Katiar' with a specific date of birth is unique. Your audit must account for these combinations.
Overhaul the Consent Mechanism Under the DPDP Act, consent is paramount and must be clear, specific, informed, and unambiguous. Immediately cease reliance on verbal or blanket consent. For all existing patients, you are required to issue a notice informing them of the personal data you currently hold. For all future data collection, you must implement a mechanism to obtain explicit consent for a clearly defined purpose. Consent to share data with a pathology lab for a blood test cannot be used to justify sharing that same data for any other purpose.
Implement Secure Systems and Cease Informal Practices Mandate the immediate cessation of using non-compliant and insecure tools for handling patient data. This means an absolute stop to using personal WhatsApp accounts, personal Gmail, and insecure Excel or Google Sheets. Invest in secure, compliant communication channels and devices that are under your organization's control, such as a secure health information management system or enterprise-grade communication tools with robust access controls and audit trails.
Prioritize Employee Training and Awareness Your employees are your first line of defense. It is critical to implement a mandatory and recurring training program for all staff, from last-mile caregivers to back-office administrators. This training must cover the fundamentals of the DPDP Act, the extreme sensitivity of patient health information, and the severe personal and professional consequences of data breaches. Staff must be educated on why their actions matter and how to handle data responsibly, transforming them from a potential liability into a compliance asset.
Implementing these measures is not just a defensive necessity; it is a strategic investment that can redefine your organization's position in the market.
6.0 Conclusion: Transforming Compliance from a Burden to a Differentiator
While the conversation around the DPDP Act is often dominated by risk and penalties, a forward-thinking perspective reveals a significant opportunity. Proactive compliance is not merely a legal burden; it is a powerful business enabler that can become a core differentiator in an increasingly data-aware market.
In the home healthcare sector, trust is the ultimate currency. An organization that can confidently and transparently state, "We protect your health and your privacy both," sends a powerful trust signal to patients and their families. This is not a passive benefit; it is an active marketing tool. In a crowded market, the ability to guarantee data privacy becomes a unique selling proposition that builds patient loyalty and justifies premium service.
Furthermore, robust data privacy practices directly impact B2B partnerships. As the entire healthcare ecosystem becomes more regulated, larger organizations like hospitals, pathology labs, and insurance companies will demand compliance from their partners to mitigate their own risk. A home care provider with a mature data privacy framework is a far more attractive and less risky partner. This not only secures existing relationships but also opens doors to new business opportunities, effectively future-proofing the organization's growth.
Ultimately, proactive DPDP compliance is not about avoiding fines. It is about building a resilient, trustworthy, and market-leading home care brand for the future—one that is prepared for the next wave of digital transformation and poised to earn the lasting confidence of patients and partners alike.
HOMECARE ASSOCIATION OF INDIA
WHAT HCAI IS DOING ABOUT IT
• 5 virtual convenings completed with operators, clinicians, and policy voices.
• HCAI Charter released on 15 August.
• Charter sets principles on consent, data minimisation, caregiver access, and accountability.
.Homecare Association of India - Charter
HCAI is open, collaborative, and builder-led.
Apply for Membership at https://docs.google.com/forms/d/e/1FAIpQLSdID2atG47kNGSHwoano1nXTYjq375c7tfPdt6pGyWVJ2_Yfw/viewform?pli=1
